Body mass index, or BMI, is a number that is frequently used by healthcare professionals to classify individuals as underweight, overweight, or obese. It’s also used by insurance companies as a metric for assessing risk – if you have a higher BMI, you may not qualify for the best life insurance policy. Recently, it’s come under fire as a metric for health. What exactly is it, and is it useful?
BMI was first coined in a 1972 paper by Ancel Keys. Ancel Keys was a health researcher who is most famous for his 7 nation study, in which he advocated for a Mediterranean style diet. His research led to the low fat movement of the 20th century. Now, it’s possible his findings were misconstrued and that the food manufacturers are to blame for pumping all sorts of chemicals into low fat foods which in turn made them unhealthier than they would have been without manipulation. Still, it’s difficult to move past the fact that his 7 nation study was based on 7 countries he selected out of the 22 for which he had data.
Back to BMI – in his 1972 paper, Keys argued that BMI was a great method of viewing obesity in a given population – it was designed for a statistical analysis, rather than for individual analysis, which is how it is frequently applied. BMI is calculated by taking mass and dividing it by the square of an individual’s height:
BMI = Mass (kg) = Mass (lbs) x703
Height(m)2 Height (in)2
Currently, individuals with a BMI of 25 or higher are considered overweight. At 30 and higher, an individual is considered obese. From 1972 until 1998, 27.8 was the cutoff to be considered overweight. While this change could certainly influence the current US numbers indicating that we have an obesity epidemic, it would be naïve to suggest that it’s the only factor.
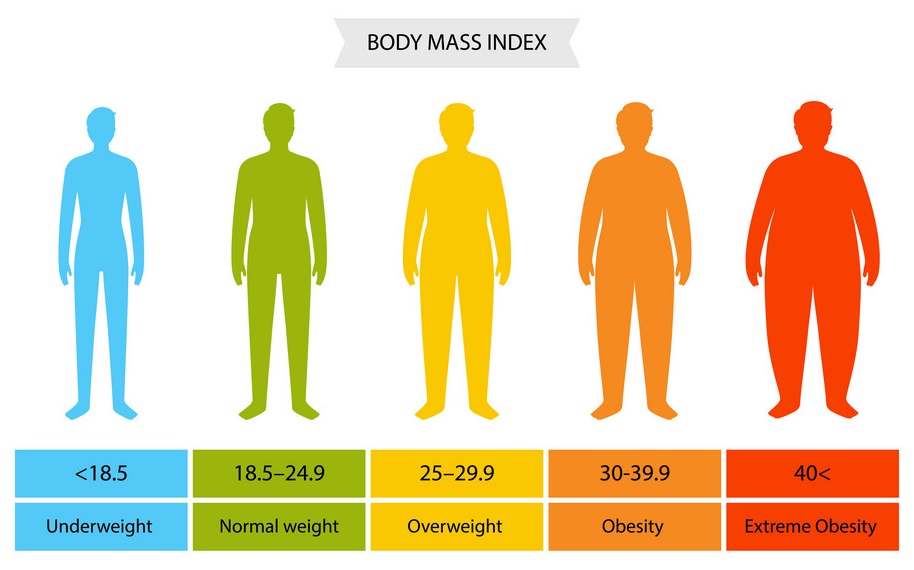
Now, on to the problems with BMI. Hopefully the first one is obvious – since height squared is the denominator, taller individuals who are proportionally the same as shorter individuals have a higher BMI. Additionally, the method was originally proposed to gauge the health of sedentary populations, rather than active ones. This means it was designed for a more adipose population – the presence of muscle mass can skew the measurement.
As many of us at Viking Athletics are aware, it is very possible to have a statistically normal, or even low bodyfat percentage, and still be considered overweight or obese based on BMI. So, the measurement is inaccurate in extremely athletic individuals. At extreme ends of the spectrum – namely extremely skinny or extremely adipose individuals, the number is also skewed.
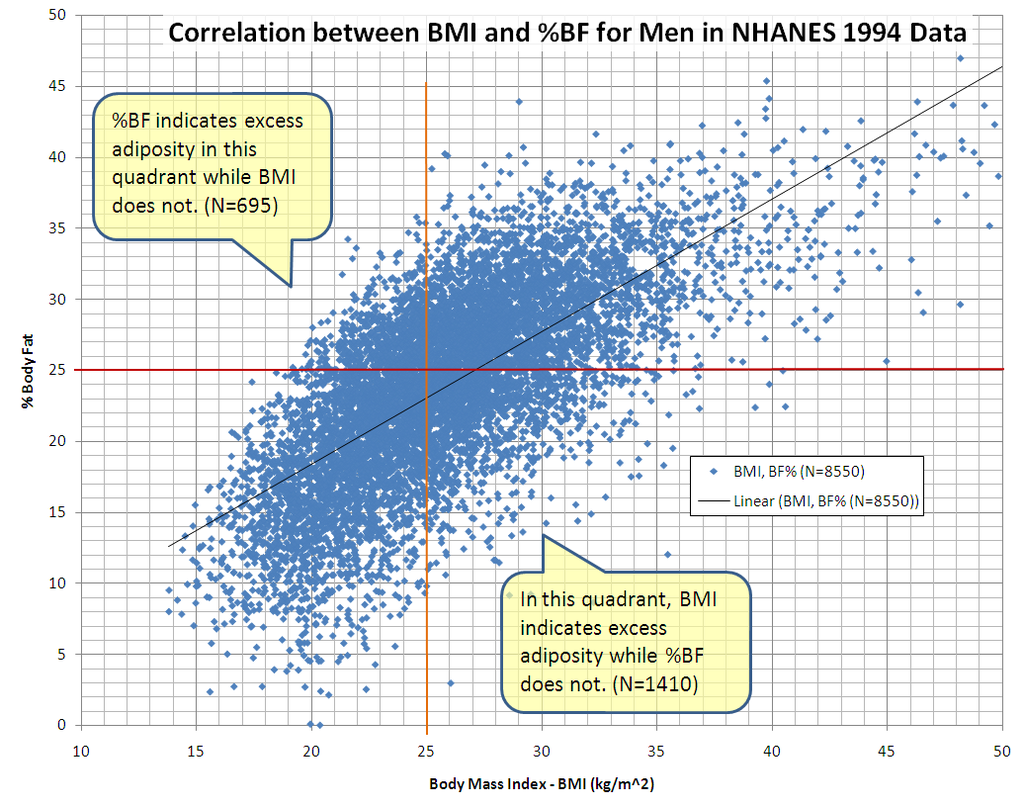
Before dismissing BMI completely, it is worth noting that it is still a good indicator for risk of heart attack. Many body builders, though extremely lean, have high BMIs, and suffer from heart trouble. At the end of the day, your heart doesn’t care if it’s pumping blood to muscle or adipose tissue – the bigger the individual, the harder the heart must work. So, regardless of other factors, if you have a high BMI, you should be doing some steady state cardio for heart health to mitigate your risk.
At the end of the day, it’s important to remember that BMI was designed to analyze populations, not individuals. And while it has its limits with subsets of the population, it’s still useful from a statistical standpoint. When it comes to individual use, BMI is only a small part of the picture. Body fat percentage, blood markers, and visceral fat level are more important. While we can’t do blood work for you at the gym, we can measure BMI, body fat percentage, basal metabolic rate, and visceral fat. If you’re ever interested, book an InBody appointment with us! Otherwise, keep in mind that your body mass index doesn’t tell the whole story, and don’t lose any sleep over it. See you in the gym.
